Healthcare infrastructure projects are more than steel beams and mechanical systems – they are investments in community well-being, operational excellence and patient outcomes.
At STV, program delivery for these projects is grounded in pairing technical expertise with an understanding of how healthcare spaces are actually used by patients, clinicians and staff. This balance is especially crucial in complex diagnostic environments like MRI suites, where innovation must be carefully managed alongside safety, coordination and long-term resilience.
Serving one of the most diverse and dynamic communities in Brooklyn, Brookdale University Hospital Medical Center advanced its diagnostic capabilities with a new state-of-the-art magnetic resonance imaging (MRI) suite. Delivered within an active hospital environment, the project required navigating constrained existing infrastructure, coordinating across multiple stakeholder groups and executing highly time-sensitive installation sequences – all while maintaining patient safety and uninterrupted care.
As part of STV’s ongoing program management support for the One Brooklyn Health system, the MRI suite reflects a broader commitment to strengthening access to advanced diagnostic care through thoughtful planning, collaboration and patient-centered design. In this conversation, STV’s Annfiera Jarvis-McPherson, senior project manager, and David Wilklow, project director with the firm’s program and construction management team, share insights on delivering complex healthcare projects – from managing technical risks to making design decisions that support both clinical performance and patient comfort.

Why are projects like the Brookdale MRI suite significant investments for community-based hospitals?
Annfiera Jarvis-McPherson: Advanced imaging technology like Brookdale’s MRI significantly enhances diagnostic capabilities, enabling earlier and more accurate detection of a wide range of conditions. For underserved communities in Brooklyn, having timely access to diagnostics can directly affect patient outcomes and continuity of care. Projects like this expand a hospital’s ability to serve patients locally – including those with mobility challenges or complex health needs – while supporting more equitable access to advanced care. Strong program management helps verify that investments focus on what matters most: upgrading critical equipment, integrating new technology and improving patient flow and operational efficiency.
David Wilklow: From an infrastructure perspective, MRI projects are major operational investments. These systems are highly specialized and extremely sensitive, requiring precise coordination across building systems, schedules and safety protocols. When delivered successfully, they enable hospitals to maintain advanced imaging capabilities on site, reducing delays, enhancing care coordination and supporting faster, better-informed clinical decisions – rather than sending patients elsewhere for essential diagnostics.

What makes MRI installations uniquely complex, especially within active hospitals?
David Wilklow: An MRI is a powerful magnet that needs to be delivered super-cooled and installed within a very narrow window. Everything must be ready when it arrives: chillers, HVAC, power, shielding and access routes. Delays can cause liquid nitrogen to boil off, creating serious safety risks and costly setbacks. Even when powered down, an MRI remains magnetic, which is why strict controls, specialized materials and experienced contractors are essential. Something as small as a misplaced tool can become dangerous in seconds.
MRI suites are among the most complex rooms in a hospital. They require additional structural support for the 20,000-pound weight, 480-volt power, separate HVAC on emergency power, a complex venting system and radio frequency shielding for the MRI vault.
Annfiera Jarvis-McPherson: Healthcare construction also comes with layers of regulatory complexity, including requirements from the Department of Health, the Joint Commission and local authorities. On top of that, you’re working with specialized spaces like operating rooms, labs and radiology suites – all with advanced mechanical, electrical and plumbing needs. Many of these projects take place in occupied facilities, which means every phase must be carefully planned and coordinated to avoid disrupting daily hospital operations.
How does modernizing diagnostic spaces improve both patient care and the patient experience?
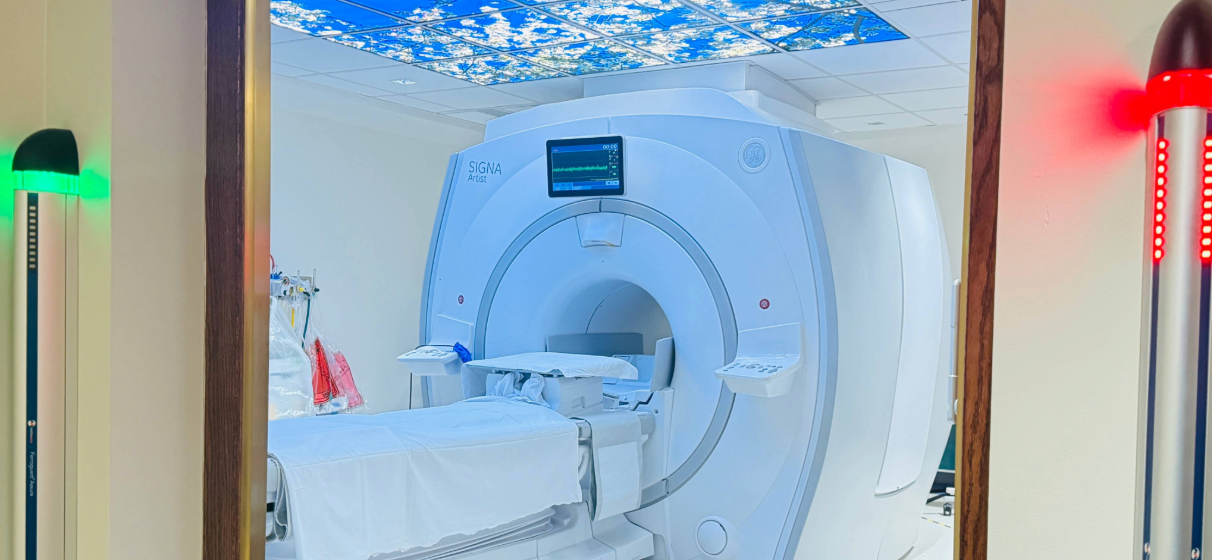
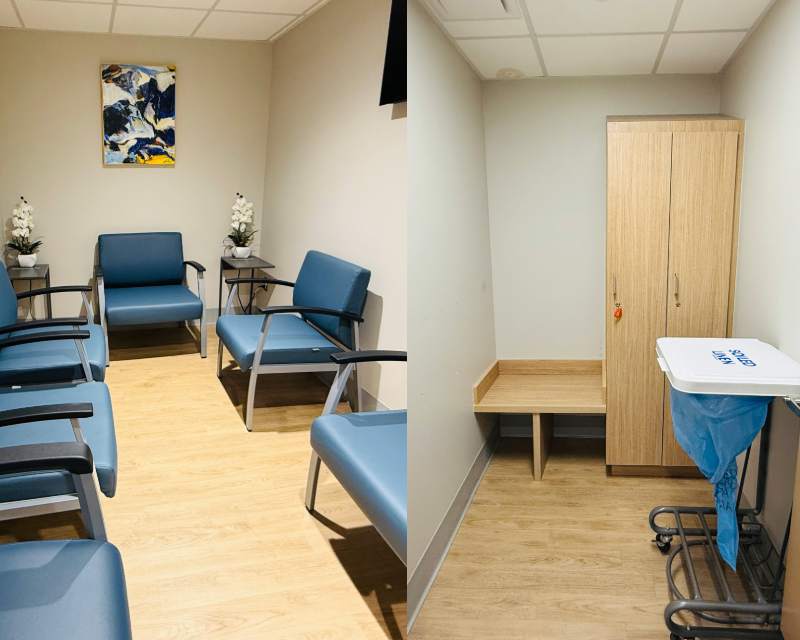
Annfiera Jarvis-McPherson: Patient experience was never an afterthought on this project – it was part of every conversation. Beyond the technology itself, we paid close attention to how the space would feel for patients. From the illuminated ceiling mural to the calming color palette in the MRI suite and reception areas, every design choice was made with patient comfort in mind. Imaging can be intimidating, especially for patients who are already anxious and small details can make a meaningful difference in helping people feel more at ease.
David Wilklow: Design has a real impact on how people experience healthcare spaces. Lighting, materials, colors and acoustics all influence comfort and perception. Even subtle decisions, such as avoiding harsh colors or using seamless flooring that supports infection control, can enhance both safety and the overall patient experience without drawing attention to themselves.

Why is early planning so critical in complex healthcare projects?
David Wilklow: For imaging projects, early decisions are critical to avoid construction delays and cost increases. Once an MRI room is built, changes become extremely difficult and expensive. Even adding a single outlet later can compromise shielding and trigger rework across multiple systems. Reviewing details early with hospital medical and administration staff and facilities teams helps protect the schedule, budget and long-term performance of the space.
Annfiera Jarvis-McPherson: Early planning also allows teams to anticipate risks and develop contingency strategies before issues arise. Regular assessments of existing infrastructure, clear documentation and early approvals help keep everyone aligned, even when leadership or priorities change over time.
What key lessons from Brookdale will shape future healthcare projects?
David Wilklow: One of the biggest lessons from Brookdale is the importance of fully understanding existing infrastructure before design begins. In active hospitals, there are often hidden conditions, such as risers, utilities and systems serving critical areas, that can quickly impact scope, schedule and cost if they aren’t identified early. Capacities of the existing systems must be confirmed before the design is finalized. At Brookdale, we had to rethink structural solutions on the fly to avoid disrupting patient rooms and essential building systems. That experience reinforced the value of early investigation, close coordination and creative problem-solving. Looking ahead, successful healthcare projects will continue to rely on this upfront diligence, paired with patient-centered design, digital integration and efficient, sustainable materials that support long-term flexibility.
The MRI delivery path must be carefully planned, often requiring structural reinforcement. Large openings into the building are needed. All deliveries require a crane, which requires logistics planning and special permits.
How does strong collaboration and client partnership influence project success?
Annfiera Jarvis-McPherson: Healthcare projects succeed when collaboration becomes a true partnership built on trust. At Brookdale, I worked closely with hospital leadership, radiology staff and facilities teams throughout the project, including Wayne Jordan, director of radiology. From the beginning, Wayne had a clear understanding of the department’s needs – particularly regarding the MRI system upgrade – and he trusted our team to help translate those needs into practical, long-term solutions.
That trust made a real difference. It allowed for open, honest conversations and quick decision-making as challenges arose. We worked through details together – from technology selection to workflow and safety considerations – always keeping in mind how the space would function day to day for staff and patients. Bringing clinical and operational teams into the process early helped us stay proactive, coordinate carefully and minimize disruption during installation.
If there’s one takeaway about delivering healthcare projects, what would it be?
Annfiera Jarvis-McPherson: Clear communication and collaboration are essential. When everyone stays focused on the needs of patients and end users, projects are better positioned to succeed.
David Wilklow: Healthcare construction doesn’t happen in isolation. Respecting the people, systems and patients already in the building – while planning for what comes next – is what ultimately defines success.