Delivering high-acuity healthcare projects in dense urban environments requires more than technical coordination – it demands an understanding of how design decisions affect clinical operations, patient experience and constructability in real time.
At Brookdale University Hospital Medical Center, this perspective is shaping ongoing improvements as part of the One Brooklyn Health System’s (OBHS) $664 million transformation to modernize and integrate care across central and eastern Brooklyn. These investments are focused on strengthening patient safety, improving the care experience and aligning aging facilities with the realities of contemporary healthcare delivery.
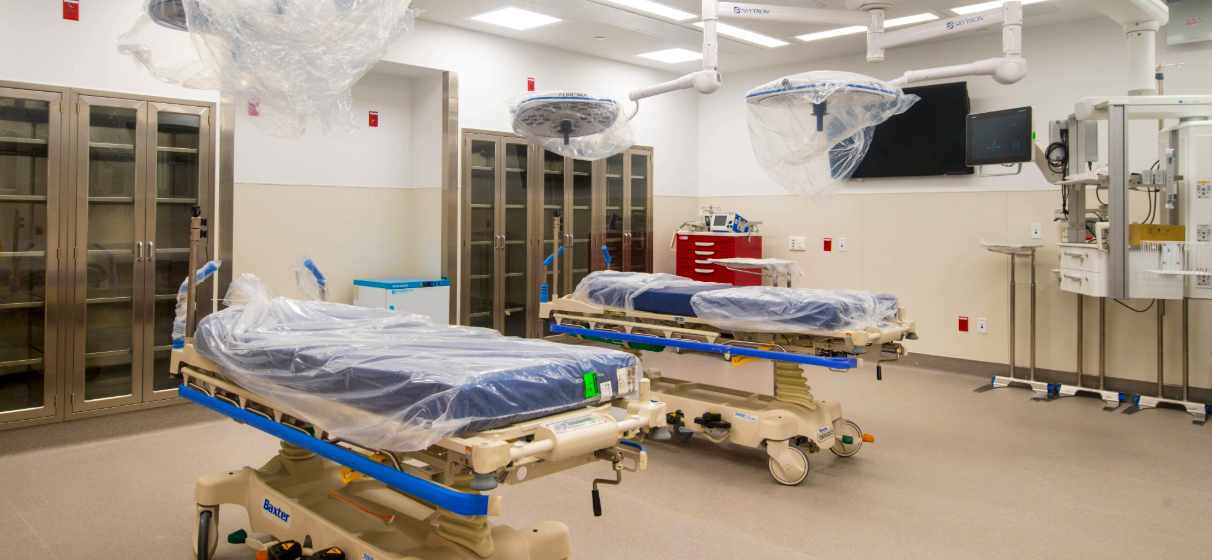
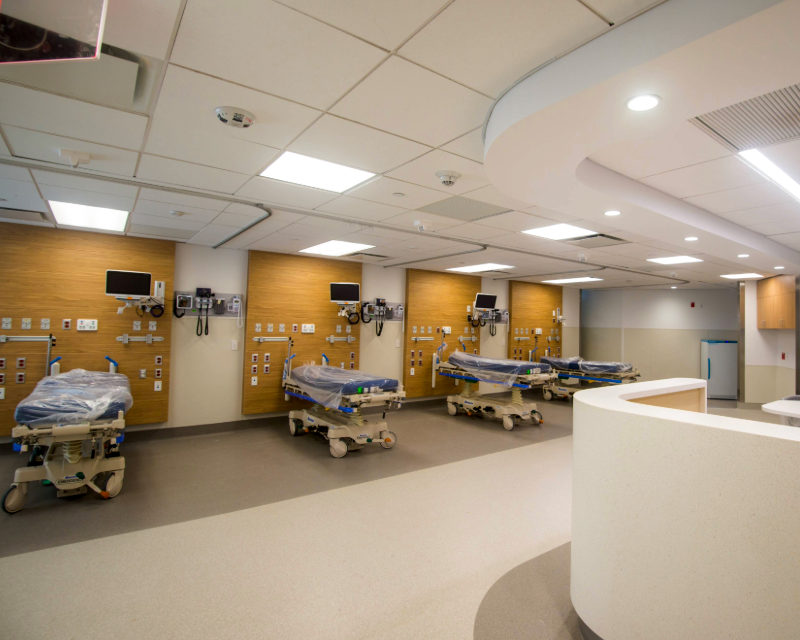
In fast-paced settings like Brookdale’s Emergency Department, design considerations extend well beyond aesthetics. From a program and construction management standpoint, they influence how teams evaluate sightlines that support faster clinical response, patient-flow pathways that reduce bottlenecks and trauma-informed strategies – such as noise control, lighting and material selection – that contribute to calmer, more supportive environments for patients and families. Behavioral health spaces connected to Comprehensive Psychiatric Emergency Program (CPEP) functions add another layer of complexity, requiring close coordination to balance safety, dignity and patient comfort within an active hospital setting.
To explore how design-informed thinking supports effective project delivery, we spoke with Arta Gashi, healthcare project manager within STV’s program management and construction management operating group. Drawing on her architectural background, Gashi brings a unique lens to her role – helping translate design intent into practical, constructible solutions that support clinical needs, schedule certainty and overall program success at one of Brooklyn’s busiest healthcare hubs.
1. What guides your overall approach to healthcare project management within One Brooklyn Health?
My path into healthcare project management began in Kosovo, where I studied architecture and urbanism. When I moved to the United States, my work across both design and government exposed me to the healthcare sector and the unique complexity of hospital environments. What keeps me in this field is the deep sense of purpose, knowing that every planning, design, or coordination decision ties directly to patient care, community well-being and the overall safety and functionality of a healthcare facility.
That foundation shaped my approach at Brookdale. Through my PM/CM work, I focus on thoughtful, purpose-driven design that strengthens clinical workflow, supports care teams and improves the experience of patients who rely on these facilities every day.
2. How does collaboration with clinical, design and construction teams shape your work?
For me, collaboration starts with listening. Each project brings together nurses, physicians, administrators, contractors and facilities staff – all with essential insights about how a space must function. Clear communication early in the process builds trust and helps ensure that our design and operational decisions align with the needs of both patients and staff.
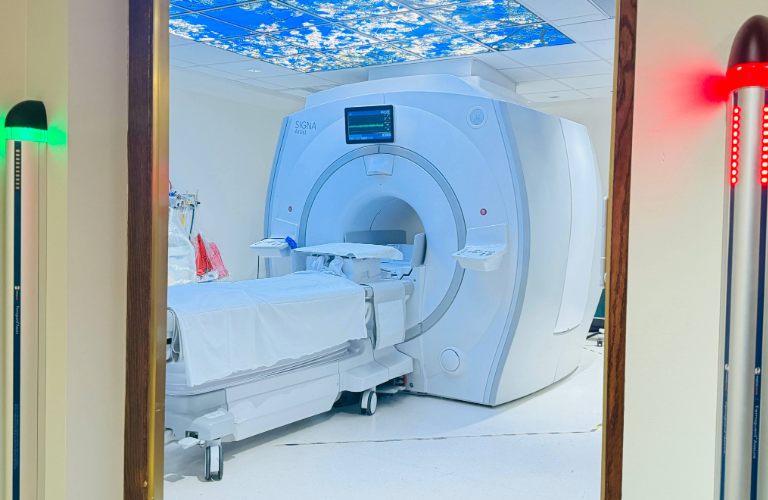
I’ve seen how powerful that collaboration can be across Brookdale’s capital program. For example, during the MRI suite project completed in 2024, Annfiera Jarvis-McPherson and David Wilklow demonstrated how trust, interdisciplinary teamwork and respect for active hospital operations are essential to delivering complex improvements in an occupied healthcare facility.
3. Can you share a recent moment that captures the impact of your work — particularly in the Emergency Department?
One moment that has stayed with me was during a behavioral health upgrade in the Emergency Department. When staff toured the renovated space for the first time, someone said it felt like “the Taj Mahal compared to what we had before.” Hearing that reinforced how transformative a well-designed environment can be – not just for patient dignity and safety, but for staff morale and their ability to deliver compassionate, high-quality care.
In addition, my work has extended to behavioral health areas connected to CPEP-related functions. These spaces require a specialized design lens – balancing safety, dignity and patient comfort. Trauma-informed design plays a central role: controlling noise, minimizing visual overstimulation, and supporting calmer, more grounded experiences for patients and families during acute behavioral health crises.
4. What makes healthcare environments – especially high‑acuity spaces – so uniquely challenging and meaningful to design for?
Healthcare facilities operate around the clock, so every design and construction decision affects safety, clinical workflow, infection control and day-to-day operations. The stakes are incredibly high. The rigor of healthcare codes and standards elevates the responsibility of my role. I’m contributing to spaces that protect life, support clinical teams and maintain critical hospital functions.

5. What advice would you give to someone entering healthcare project management?
No one enters this field knowing everything – and that’s okay. I always encourage emerging professionals to stay curious, ask questions and seek mentorship. Healthcare is both complex and deeply human, and the best way to grow is to remain open to learning.
When you value collaboration and keep patients at the center of every decision, the work becomes incredibly rewarding.